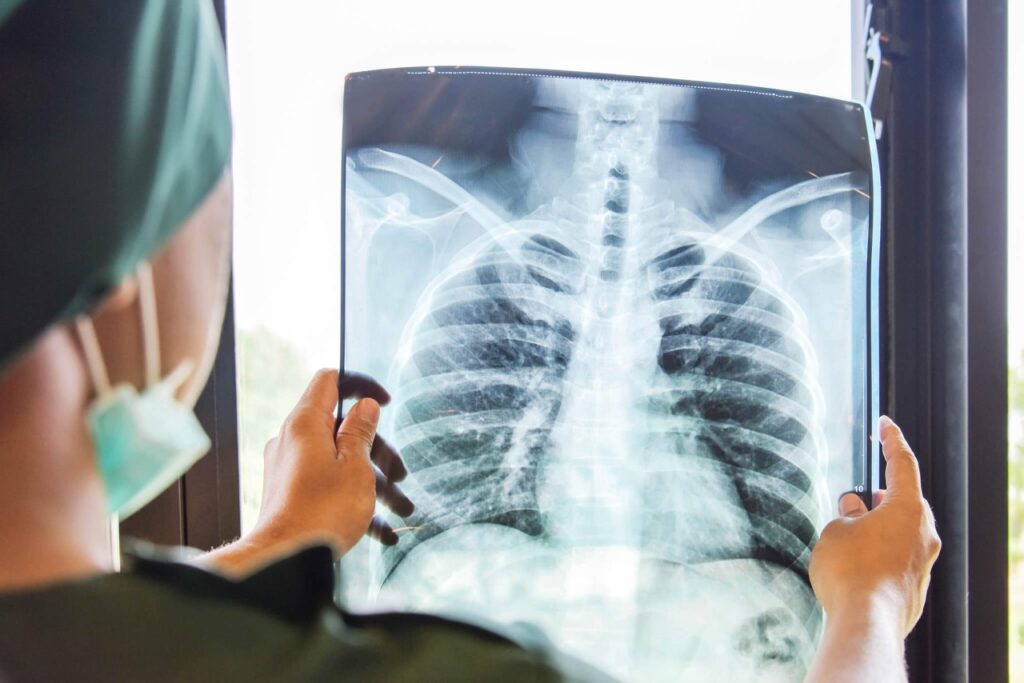
If you have cystic fibrosis or bronchiectasis, you are more likely to get chest infections. Infections affecting the lung are a spectrum from a simple upper respiratory tract ‘cold’ to a life-threatening pneumonia. Luckily, most are mild and many are preventable. The lungs are highly evolved to quickly wrap up and expel foreign viruses, bacteria and particles using white blood cells and ‘hair’ cells which move unwanted material up to the throat (like an escalator). Bronchiectasis leaves you with damaged airways which cannot always fend off germs. The airways are wider, produce more mucus and the white blood cells many not be as mobile or efficient. The hair-like cilia cells are not able to move germs out of the lung if they are covered in sticky mucus. The factors allow bacteria and viruses to get a hold and stick around.
What should I look for?
Typical symptoms such as fever or chills many be absent. Many people notice worsening cough, an increase in the amount of mucus they produce. The mucus may be stickier, foul smelling or darker in color. You may even see streaks of blood in it (blood = inflammation = infection). More severe infections may leave you breathless with exercise or even normal activity. Chest pain is rare but can occur if infection is close to the edge of the lung.
How can I protect myself from getting infections?
The COVID-19 pandemic in 2020 focused our attention on how viruses spread. Many of the same concepts apply to bacteria which can spread from one person with bronchiectasis to another very easily. Most germs (viruses and bacteria) spread through contact or the droplet route. Spreading through contact is the transfer of the germ through surfaces, onto hands and into noses and mouths (for example door handles, water bottles, shaking hands). When someone coughs, any germs in the throat or lungs gets catapulted into the air in tiny mucus droplets. If you breathe these in, the germ could end up in your lungs and multiply its new home.
Make sure you avoid other people who have cold symptoms, wear a mask in crowded public places and wash your hands frequently with soap and water. Alcohol based hand sanitizer is an alternative. Ask your doctor about vaccinations against flu and pneumococcus (pneumonia shot). The flu shot is required every year and is available from September onwards. Vaccination against pneumococcus requires only 2 injections – ask your doctor for more information.
What if I do get an infection?
It’s really important to speak to your doctor sooner rather than later. A lingering infection in people affected by bronchiectasis can permanently worsen your lung function so early signs of infection should be aggressively treated with antibiotics. Having a pulmonologist who knows your history will ensure you receive antibiotics specific to you. Urgent care clinics and emergency rooms are important resources if you need immediate attention but do not have the expertise for bronchiectasis and cystic fibrosis. It is harder to achieve adequate antibiotic levels in bronchiectatic lungs and more unusual bacteria which infect people with bronchiectasis need more than just a Z-pack. For these reasons it is typical for people with cystic fibrosis and bronchiectasis to be treated with longer courses of antibiotics, higher doses and even combination therapy with two drugs.
Resistant bacteria
When lungs become damaged, their ability to fight off germs becomes compromised. Over time, living with cystic fibrosis and other forms of bronchiectasis increases your risk of becoming ‘colonized’ with bacteria which are resistant to standard first line antibiotics. Colonization is where bacteria live and multiply in your lungs and are unable to be fully eradicated. We often say someone is colonized if we keep growing the same bacteria from repeated sputum samples over months. With some bacteria it is hard to known if they are living in your lungs innocently or if they are slowly damaging your lungs over years. For this reason, monitoring your symptoms and getting frequent breathing tests at your pulmonologist’s office is really important. At the least we recommend visits every 3 months where we do spirometry (breathing tests) and ask for a sputum sample if you are able to provide one.
Why do I keep getting episodes of bronchitis?
Good question. If you are someone who keeps getting chest infections or just cannot shake a cold, it could be one of the following reasons.
- Maybe it is not an infection at all. It’s always important to consider alternate diagnoses if your symptoms are not settling after adequate treatments. Your doctor should be proactive to ensure additional tests are done to investigate persisting symptoms.
- Are you on the right antibiotic? Rather than comparing antibiotics using terms like ‘stronger’ or ‘more potent’, it is important to consider which types of bacteria the drug covers. Effective treatment only happens when the right antibiotic is given at the right dose for the right length of time. Remember viral infections also causes infections or flare ups and antibiotics have no effect on viruses.
- Are you taking your treatments properly? Doctors and nurses often forget to check how you use your inhalers or nebulizers so please ask for a demonstration! Pay attention to whether any medications by mouth should be taken with food or not – this can affect how easily the drug is absorbed into the bloodstream.
- Is your airway clearance optimized? If sputum is not removed from the lungs it acts as a nidus for new infection by creating a warm, wet place for bacteria to incubate and multiply. Ask your doctor about ways to improve your airway clearance or click here.
- Still coughing weeks later? Airway infections cause a lot of airway inflammation. Even after all the viruses and bacteria have been killed and removed by your white blood cells, your lungs are damaged and will take time to heal. That period can take a long time and your lungs may be very sensitive or ‘hyperreactive’ during this time. It can be very normal for a cough to persist weeks after a simple cold.
- Is there an irritating germ in your lungs we don’t yet know about? This should be in the back of your doctor’s mind. If someone is not responding to therapy the expected way, it is possible that there is a deep-rooted infection which will not be identified from sputum samples. In select cases we perform a bronchoscopy (fiberoptic camera in the lungs) to get deep washes from the lung to look for unusual bacteria, viruses or even fungus.